Are you experiencing any health concerns after a hysterectomy 20 years later?
Then, it is essential to seek professional help.
One concern that may arise is unexpected bleeding. It is a sign that needs prompt medical attention. Post-hysterectomy bleeding can be alarming. However, it is often manageable with the proper medical intervention.
A study conducted by the Women’s Health Initiative found that nearly 10% of women experience symptoms or complications several years after hysterectomy that may require medical attention.
At Bloom IVF Centre in India, Dr. Hrishikesh Pai offers comprehensive guidance and care in such cases. Dr. Pai is one of the leading gynecologist and IVF doctor in India. He emphasizes the importance of seeking medical advice if you experience post-hysterectomy bleeding.
In this blog, we aim to provide valuable insights and solutions for those facing challenges years after hysterectomy.
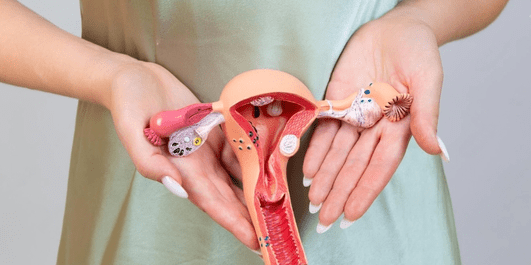
So, what exactly is a hysterectomy? Let’s find out:
Overview of Hysterectomy
Hysterectomy involves the removal of the uterus and sometimes the cervix and other surrounding tissues. These may include uterine fibroids, endometriosis, chronic pelvic pain, or cancer. It is one of the most performed surgeries among women, especially those in their 40s and 50s.
Modern surgical techniques have made hysterectomies safer and less invasive. Laparoscopic surgery is one such minimally invasive option. It helps patients recover more quickly.
Deciding to undergo a hysterectomy is a personal and often complex choice. Women must talk with their gynecologist about all options and outcomes. This helps make a well-informed decision. It includes understanding the surgery’s implications on their health, lifestyle, and mental well-being.
Wondering what happens two decades after the surgery? Read on:
What to Expect 20 Years After Hysterectomy?
20 years post-hysterectomy, women may experience long-term effects of the surgery along with the natural aging processes. These can lead to significant changes in their bodies. Understanding what to expect during this time frame is essential, as each individual’s experience can vary.
Primarily, removing the uterus ends menstrual cycles and the possibility of conception permanently. If the ovaries were left intact during the hysterectomy, menopausal symptoms might not start right away. It will begin as per their natural menopausal timing.
The symptoms may include hot flashes, mood swings, and changes in libido. It results from the natural aging of the ovaries. For women whose ovaries were removed with the hysterectomy, these symptoms typically start right after the surgery.
Another concern is the risk of pelvic floor disorders, which may increase with time. The absence of the uterus can lead to changes in pelvic support and function. This can lead to conditions like urinary incontinence or pelvic organ prolapse.
Maintaining a healthy lifestyle, including regular exercise, is essential to strengthen the pelvic floor muscles and mitigate these risks.
Furthermore, there are emotional and psychological aspects to consider. The impact of a hysterectomy on mental health and body image can be profound. These feelings might evolve or resurface even years later.
Regular check-ups with gynecologists and mental health professionals are crucial for comprehensive care.
Experiencing bleeding after hysterectomy 20 years later?
For expert care and guidance, schedule a consultation with Dr. Hrishikesh Pai at your nearest Bloom IVF Centre in Navi Mumbai, Delhi, Gurgaon, Indore, Lucknow, Nagpur, Kolkata, Mohali, Faridabad.
But is it normal to experience bleeding so long after the procedure? Let’s explore:
Is Bleeding After Hysterectomy 20 Years Later Normal?
Bleeding years after a hysterectomy often raises concerns among patients, and rightly so. Bleeding after hysterectomy 20 years later is not normal. It is crucial to seek immediate medical attention. This bleeding could signify various health issues, ranging from minor to more severe.
The causes of post-hysterectomy bleeding can vary. In some cases, it may be due to vaginal atrophy. It is a common condition in postmenopausal women. In this condition, the vaginal walls become thin and more prone to bleeding.
In other instances, it could be a sign of more severe issues like vaginal or endometrial cancer. It is imperative to consult a seasoned gynecologist like Dr. Hrishikesh Pai for an accurate diagnosis.
Early detection and treatment of any underlying condition are vital to managing health effectively after a hysterectomy.
What can be done to address these complications?
Treatment Options for Post-Hysterectomy Complications
For post-hysterectomy issues like unexpected bleeding or similar symptoms 20 years later, a personalized and informed treatment plan is crucial. Here are several key options to consider:
1. Medical Evaluation:
Always begin with a thorough medical evaluation. This includes consultation with a gynecologist specializing in post-hysterectomy care.
2. Hormonal Therapy:
For hormonal imbalances, Hormone Replacement Therapy (HRT) is often a go-to solution. It helps in managing symptoms like hot flashes, mood swings, and vaginal dryness. However, HRT isn’t suitable for everyone. Discussing the risks and benefits with your doctor is crucial.
3. Non-Hormonal Medications:
For those who can’t use HRT, non-hormonal medications might be an option. These can include antidepressants for mood swings or vaginal moisturizers for dryness.
4. Lifestyle Modifications:
Simple lifestyle changes can make a big difference. Regular exercise, a balanced diet, and stress management techniques can improve overall health. They can also help alleviate some post-hysterectomy symptoms.
“Each patient’s situation is unique. Open discussion with your doctor is essential to determine the most suitable treatment plan,” explains Dr. Hrishikesh Pai, a reputed gynecologist and IVF specialist in India.
“Staying informed and proactive in your health journey is critical to managing life after a hysterectomy.”
Prevention is key, but how? Let’s find out:
How Can We Prevent Post-Hysterectomy Complications?
Preventing post-hysterectomy complications is crucial for maintaining long-term health and well-being. Here are key strategies to help reduce the risk of issues arising years after the surgery:

1. Regular Health Check-Ups:
Staying in touch with your gynecologist is vital. Regular check-ups can help in early detection and management of any post-hysterectomy complications.
2. Healthy Lifestyle Choices:
A balanced diet, regular exercise, and maintaining a healthy weight are essential. These habits contribute to overall well-being and can reduce the risk of complications.
3. Pelvic Floor Exercises:
Strengthening your pelvic floor muscles through exercises can help prevent urinary incontinence. It is a common concern after hysterectomy.
4. Stress Management:
Stress can have a profound impact on your physical health. Stress-reducing activities like Yoga, meditation, or mindful breathing can be beneficial.
5. Educate Yourself:
Being aware of the long-term effects of a hysterectomy is essential. It helps you stay alert to any changes in your health.
6. Open Communication:
Discussing any unusual symptoms, like bleeding after a hysterectomy, with your doctor is critical. Don’t hesitate to report even minor issues.
Consult with specialists like Dr. Hrishikesh Pai for detailed guidelines and personalized advice. Their expertise in women’s health post-hysterectomy is invaluable.
Not sure when to see a doctor? Here’s some guidance:
When to Consult a Doctor?
After a hysterectomy, being vigilant about your health is crucial. But when should you consult a doctor? It is essential to listen to your body and recognize signs that may warrant a visit to a healthcare professional.
1. Unexpected Bleeding:
If you experience bleeding years after a hysterectomy, it is a sign to seek medical advice. Bleeding after a hysterectomy, especially 20 years later, is unusual and should not be ignored.
2. Persistent Pain or Discomfort:
Any persistent pain, discomfort, or unusual symptoms in the abdominal area should prompt a consultation. These symptoms could indicate various health issues that require medical attention.
3. Changes in Bladder or Bowel Habits:
Significant changes in your bladder or bowel habits can cause concern. This includes frequent urinary infections, incontinence, or bowel changes.
4. General Health Concerns:
If you have concerns about hormone therapy, menopausal symptoms, or general well-being, it is wise to discuss these with your doctor.
It is always better to err on the side of caution. Routine check-ups ensure you stay ahead of any potential health issues.
Taking proactive steps in managing your health is vital to a better quality of life post-hysterectomy.
Conclusion
In summarizing the journey 20 years post-hysterectomy, it is evident that this milestone brings unique challenges and concerns. These may include the possibility of post-hysterectomy bleeding. Patients should be proactive about their health. They should recognize that any changes in their body require attention and may need medical evaluation.
Consulting seasoned experts like Dr. Hrishikesh Pai at Bloom IVF Centre in Mumbai can offer expert guidance and care. Dr. Pai’s extensive experience in women’s health reassures those navigating post-hysterectomy life.
FAQs:
How does age at the time of hysterectomy affect long-term outcomes?
Younger age at hysterectomy may influence the range and intensity of long-term symptoms.
Can a hysterectomy affect sexual health in the long term?
Yes, it can. Changes in libido or vaginal health post-hysterectomy are possible. However, we can manage them with medications.
Is osteoporosis a risk after a hysterectomy?
There is an increased risk, especially if the ovaries are removed. It can affect the bone density.
Are urinary issues common decades after a hysterectomy?
Urinary incontinence or infections can occur but are manageable with proper medical care.
Can a hysterectomy lead to weight gain years later?
Hormonal changes post-hysterectomy can contribute to weight fluctuations.


Your point of view caught my eye and was very interesting. Thanks. I have a question for you.
Please ask