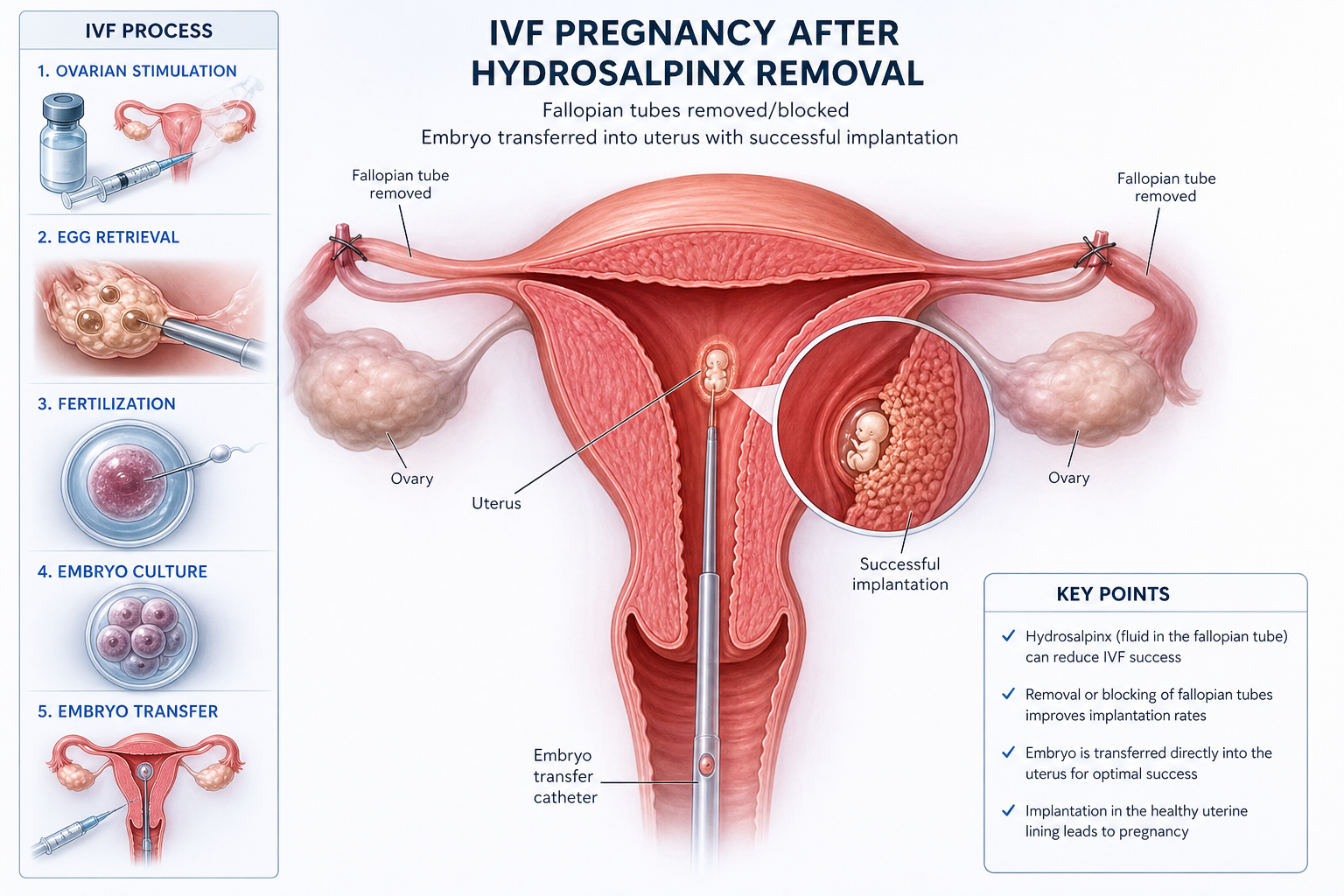
Pregnancy after hydrosalpinx removal becomes significantly more likely once the blocked, fluid-filled fallopian tube is excised or clipped. Studies show IVF success rates improve significantly after surgical removal because the toxic fluid no longer leaks back into the uterus. Natural conception is possible in select cases too.
According to Dr. Hrishikesh Pai, IVF specialist in India, “Removing or clipping a hydrosalpinx before IVF is one of the most predictable ways to improve implantation rates. The fluid inside damaged tubes is embryotoxic, and clearing it out gives the embryo a real chance to settle.”
How Does Hydrosalpinx Removal Improve Pregnancy Chances?
Hydrosalpinx is a condition where the fallopian tube swells with fluid due to blockage, often from past infection or endometriosis. That fluid is the real problem. It seeps into the uterus, lowers endometrial receptivity, and may interfere with embryo implantation.
Removal works through three mechanisms:
Stops embryotoxic leakage: The inflammatory fluid no longer reaches the uterine cavity.
Improves endometrial receptivity: The lining recovers its natural ability to support implantation.
Improves IVF success rates: Pre-surgery rates near 17 percent jump to 30 to 40 percent post-surgery
Reduces ectopic risk: Damaged tubes increase the risk of ectopic pregnancy, and surgery helps reduce this risk.
The standard procedure is laparoscopic salpingectomy, full removal of the affected tube. Some patients qualify for tubal blockage treatment through clipping instead. Your surgeon picks the approach based on tube condition, age, and ovarian reserve.
Thinking about pregnancy after your hydrosalpinx surgery? Book a consultation with Dr. Hrishikesh Pai to create a fertility plan tailored just for you.
When Can You Try to Conceive After Hydrosalpinx Removal?
Recovery timing matters. Trying too early stresses incision sites and pelvic tissue still healing internally. Waiting too long delays your fertility window unnecessarily.
Standard timelines:
2 weeks: Light activity resumes, no intercourse, no exercise.
4 to 6 weeks: Full healing of laparoscopic ports and internal tissue.
6 to 8 weeks: Cleared for natural conception attempts if both ovaries function and the other tube is healthy.
8 to 12 weeks: Recommended waiting period before starting an IVF cycle to allow full pelvic recovery.
Patients planning IVF should schedule the cycle around 2 to 3 months after surgery. This window lets inflammation subside completely. Anyone with a history of recurrent miscarriage should also rule out other uterine factors before attempting conception.
What Are the Chances of Natural Pregnancy After Surgery?
Natural pregnancy is possible but conditional. It depends entirely on the status of the second tube, ovarian function, and partner sperm quality.
Realistic outcomes:
One healthy tube remaining: Natural pregnancy rate around 30 to 40 percent within 12 months.
Bilateral hydrosalpinx removed: Natural conception is not possible, IVF is the only path.
Age above 35: Natural rates drop sharply, IVF becomes the recommended route.
Coexisting endometriosis: Lowers natural success, may need endometriosis treatment
Male factor present: Sperm count or motility issues require ICSI or IUI regardless of tubal status.
Couples with one healthy tube and no other fertility issues often conceive within 6 months. If 12 months pass without success, IVF discussion is the next step. Don’t wait beyond that window if you’re over 35.
Planning pregnancy after hydrosalpinx surgery? Book Appointment with Dr. Hrishikesh Pai for a personalized post-op fertility plan.
What Are the Chances of Natural Pregnancy After Surgery?
Recovery isn’t just about healing the incision sites. It’s about creating an internal environment where conception can actually happen. Some habits actively work against that.
What to skip in the first 6 to 8 weeks:
Heavy lifting: Anything above 5 kg can strain pelvic tissue and disrupt healing.
Intercourse before clearance: Wait for the surgeon’s green light, usually around week 4 to 6.
Hot tubs and saunas: Elevated core temperatures stress recovering tissue.
Smoking and alcohol: Both reduce blood flow to pelvic organs and lower implantation odds.
Skipping follow-ups: Post-op ultrasounds catch silent fluid reaccumulation early.
High-impact exercise: No running, jumping, or weight training until cleared.
Self-medicating pain: Ibuprofen and other NSAIDs can interfere with implantation if taken near conception attempts.
Stay hydrated. Eat protein-rich meals to support tissue repair. Keep moving with light walks. Most patients return to full activity by week 6, but conception planning still needs surgeon clearance.
When To Contact Your Doctor
Most patients wait until something feels wrong. That’s usually too late. Certain post-surgery symptoms and fertility delays need a specialist’s eyes immediately, not a wait-and-watch approach.
Reach out without delay if you notice:
- Persistent pelvic pain: Sharp or worsening pain beyond week 2 needs imaging.
- Fever above 38°C: Could signal post-op infection requiring antibiotics.
- Heavy or unusual bleeding: Anything beyond expected light spotting deserves a call.
- No conception after 6 to 12 months: Time to evaluate IVF options based on age.
- Recurrent miscarriage: Two or more losses point to deeper investigation.
- Suspected fluid recurrence: Pelvic heaviness or bloating may indicate hydrosalpinx return.
Dr. Hrishikesh Pai, an IVF specialist in Mumbai with over 40 years of fertility experience, recommends a post-op review at 6 weeks and a fertility plan within 3 months of surgery. Early planning shapes outcomes more than any single intervention later.


